Lapatinib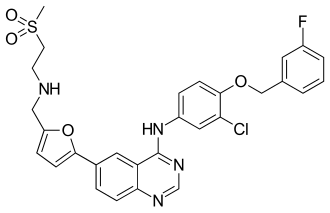 |
|
| Trade names | Tykerb, Tyverb, others |
|---|
| AHFS/Drugs.com | Monograph |
|---|
| MedlinePlus | a607055 |
|---|
| License data |
|
|---|
Pregnancy
category | |
|---|
Routes of
administration | By mouth |
|---|
| ATC code | |
|---|
|
| Legal status |
- AU: S4 (Prescription only)
- CA: ℞-only
- UK: POM (Prescription only)
- US: ℞-only
- EU: Rx-only[1]
- In general: ℞ (Prescription only)
|
|---|
|
| Bioavailability | Variable, increased with food |
|---|
| Protein binding | >99% |
|---|
| Metabolism | Liver, mostly CYP3A-mediated (minor 2C19 and 2C8 involvement) |
|---|
| Elimination half-life | 24 hours (repeated dosing), 14.2 hours (single dose) |
|---|
| Excretion | Mostly Feces |
|---|
|
N-[3-Chloro-4-[(3-fluorophenyl)methoxy]phenyl]-6-
[5-[(2-methylsulfonylethylamino)methyl]-2-furyl]
quinazolin-4-amine
|
| CAS Number | |
|---|
| PubChem CID | |
|---|
| IUPHAR/BPS | |
|---|
| DrugBank | |
|---|
| ChemSpider | |
|---|
| UNII | |
|---|
| KEGG | |
|---|
| ChEBI | |
|---|
| ChEMBL | |
|---|
| PDB ligand | |
|---|
| CompTox Dashboard (EPA) | |
|---|
|
| Formula | C29H26ClFN4O4S |
|---|
| Molar mass | 581.06 g·mol−1 |
|---|
| 3D model (JSmol) | |
|---|
CS(=O)(=O)CCNCc1ccc(o1)c2ccc3c(c2)c(ncn3)Nc4ccc(c(c4)Cl)OCc5cccc(c5)F
|
InChI=1S/C29H26ClFN4O4S/c1-40(36,37)12-11-32-16-23-7-10-27(39-23)20-5-8-26-24(14-20)29(34-18-33-26)35-22-6-9-28(25(30)15-22)38-17-19-3-2-4-21(31)13-19/h2-10,13-15,18,32H,11-12,16-17H2,1H3,(H,33,34,35)  Y YKey:BCFGMOOMADDAQU-UHFFFAOYSA-N  Y Y
|
 N N Y (what is this?) (verify) Y (what is this?) (verify) |
Lapatinib (INN), used in the form of lapatinib ditosylate (USAN) (trade names Tykerb and Tyverb marketed by Novartis) is an orally active drug for breast cancer and other solid tumours.[2] It is a dual tyrosine kinase inhibitor which interrupts the HER2/neu and epidermal growth factor receptor (EGFR) pathways.[3] It is used in combination therapy for HER2-positive breast cancer. It is used for the treatment of patients with advanced or metastatic breast cancer whose tumors overexpress HER2 (ErbB2).[4]
Status
In March 2007, the U.S. Food and Drug Administration (FDA) approved lapatinib in combination therapy for breast cancer patients already using capecitabine (Xeloda).[3][4] In January 2010, Tykerb received accelerated approval for the treatment of postmenopausal women with hormone receptor positive metastatic breast cancer that overexpresses the HER2 receptor and for whom hormonal therapy is indicated (in combination with letrozole).[4]
Pharmaceutical company GlaxoSmithKline (GSK) markets the drug under the proprietary names Tykerb (mostly U.S.) and Tyverb (mostly Europe and Russia).[5] The drug currently has approval for sale and clinical use in the US,[3][5] Australia,[3] Bahrain,[3] Kuwait,[3] Venezuela,[3] Brazil,[6] New Zealand,[6] South Korea,[6] Switzerland,[5] Japan, Jordan, the European Union, Lebanon, India and Pakistan.[5]
In August 2013, India's Intellectual Property Appellate Board revoked the patent for Glaxo's Tykerb citing its derivative status, while upholding at the same time the original patent granted for lapatinib.[7]
The drug lapatinib ditosylate is classified as S/NM (a synthetic compound showing competitive inhibition of the natural product) that is naturally derived or inspired substrate.[8]
Mode of action
Biochemistry
Lapatinib inhibits the tyrosine kinase activity associated with two oncogenes, EGFR (epidermal growth factor receptor) and HER2/neu (human EGFR type 2).[9] Over expression of HER2/neu can be responsible for certain types of high-risk breast cancers in women.[3]
Like sorafenib, lapatinib is a protein kinase inhibitor shown to decrease tumor-causing breast cancer stem cells.[10]
Lapatinib inhibits receptor signal processes by binding to the ATP-binding pocket of the EGFR/HER2 protein kinase domain, preventing self-phosphorylation and subsequent activation of the signal mechanism (see Receptor tyrosine kinase#Signal transduction).[11]
Clinical application
Breast cancer
Lapatinib is used as a treatment for women's breast cancer in treatment-naïve, ER+/EGFR+/HER2+ breast cancer patients and in patients who have HER2-positive advanced breast cancer that has progressed after previous treatment with other chemotherapeutic agents, such as anthracycline, taxane-derived drugs, or trastuzumab (Herceptin).
A 2006 GSK-supported randomized clinical trial on female breast cancer previously being treated with those agents (anthracycline, a taxane and trastuzumab) demonstrated that administrating lapatinib in combination with capecitabine delayed the time of further cancer growth compared to regimens that use capecitabine alone. The study also reported that risk of disease progression was reduced by 51%, and that the combination therapy was not associated with increases in toxic side effects.[12] The outcome of this study resulted in a somewhat complex and rather specific initial indication for lapatinib—use only in combination with capecitabine for HER2-positive breast cancer in women whose cancer have progressed following previous chemotherapy with anthracycline, taxanes and trastuzumab.
Early clinical trials have been performed suggesting that high dose intermittent lapatinib might have better efficacy with manageable toxicities in the treatment of HER2-overexpressing breast cancers.[13]
Adverse effects
Like many small molecule tyrosine kinase inhibitors, lapatinib is regarded as well tolerated. The most common side effects reported are diarrhea, fatigue, nausea and rashes.[3][14] Of note, lapatinib related rash is associated with improved outcome.[15] In clinical studies elevated liver enzymes have been reported. QT prolongation has been observed with the use of lapatinib ditosylate but there are no reports of torsades de pointes. Caution is advised in patients with hypokalaemia, hypomagnesaemia, congenital long QT syndrome, or with coadministration of medicines known to cause QT prolongation. In combination with capecitabine, reversible decreased left ventricular function are common (2%).[16]
Ongoing trials in gastric cancer
Phase III study designed to assess lapatinib in combination with chemotherapy for advanced HER2-positive gastric cancer in 2013 failed to meet the primary endpoint of improved overall survival (OS) against chemotherapy alone. The trial did not discover new safety signals, while the median OS for patients in the lapatinib and chemotherapy group was 12.2 months against 10.5 months for patients in the placebo plus chemotherapy. Secondary endpoints of the randomized, double-blinded study, were progression-free survival (PFS), response rate and duration of response. Median PFS was 6 months, response rate was 53% and the duration of response was 7.3 months in the investigational combination chemotherapy group compared to median PFS of 5.4 months, response rate of 39% and duration of response of 5.6 months for patients in chemotherapy alone group. Diarrhoea, vomiting, anemia, dehydration and nausea were serious adverse events (SAE) reported in over 2% of patients in the investigational combination chemotherapy group, while vomiting was the most common SAE noted in the chemotherapy group.[17]
References
- ^ "Tyverb EPAR". European Medicines Agency (EMA). 10 June 2008. Retrieved 12 October 2024.
- ^ Burris HA (2004). "Dual kinase inhibition in the treatment of breast cancer: initial experience with the EGFR/ErbB-2 inhibitor lapatinib". The Oncologist. 9 (Suppl 3): 10–15. doi:10.1634/theoncologist.9-suppl_3-10. PMID 15163842. S2CID 38907784.
- ^ a b c d e f g h i Higa GM, Abraham J (September 2007). "Lapatinib in the treatment of breast cancer". Expert Review of Anticancer Therapy. 7 (9): 1183–1192. doi:10.1586/14737140.7.9.1183. PMID 17892419. S2CID 36837880.
- ^ a b c "Breast cancer drug approved for new indication". Women's Health. 6 (2). Cancer.gov: 173. March 2010. doi:10.2217/whe.10.11. PMID 20187722.
- ^ a b c d "GlaxoSmithKline receives marketing authorisation in the EU for Tyverb (lapatinib), the first oral targeted therapy for ErbB2-positive breast cancer" (Press release). GlaxoSmithKline. 12 June 2008. Archived from the original on 15 June 2008. Retrieved 21 June 2008.
- ^ a b c "GlaxoSmithKline Reports Positive New Data On Tykerb (lapatinib) At The 2007 American Society Of Clinical Oncology (ASCO) Annual Meeting" (Press release). Medical News Today. 4 June 2007. Archived from the original on 13 April 2010. Retrieved 2 December 2008. Retrieved December 2, 2008.
- ^ Kulkarni K (2 August 2013). "India revokes GSK cancer drug patent in latest Big Pharma blow". Reuters. Mumbai, India. Retrieved 2 August 2013.
- ^ Cragg GM, Grothaus PG, Newman DJ (July 2009). "Impact of natural products on developing new anti-cancer agents". Chemical Reviews. 109 (7): 3012–43. doi:10.1021/cr900019j. PMID 19422222.
- ^ Wood ER, Truesdale AT, McDonald OB, Yuan D, Hassell A, Dickerson SH, et al. (September 2004). "A unique structure for epidermal growth factor receptor bound to GW572016 (Lapatinib): relationships among protein conformation, inhibitor off-rate, and receptor activity in tumor cells". Cancer Research. 64 (18): 6652–6659. doi:10.1158/0008-5472.CAN-04-1168. PMID 15374980.
{{cite journal}}: CS1 maint: overridden setting (link)
- ^ Rodriguez A (April 2008). New type of drug shrinks primary breast cancer tumors significantly in just six weeks; research provides leads to a new target in cancer treatment – the cancer stem cell. Archived from the original on 26 November 2008.
- ^ Nelson MH, Dolder CR (February 2006). "Lapatinib: a novel dual tyrosine kinase inhibitor with activity in solid tumors". The Annals of Pharmacotherapy. 40 (2): 261–269. doi:10.1345/aph.1G387. PMID 16418322. S2CID 21622641.
- ^ Geyer CE, Forster J, Lindquist D, Chan S, Romieu CG, Pienkowski T, et al. (December 2006). "Lapatinib plus capecitabine for HER2-positive advanced breast cancer". The New England Journal of Medicine. 355 (26): 2733–2743. doi:10.1056/NEJMoa064320. PMID 17192538.
{{cite journal}}: CS1 maint: overridden setting (link)
- ^ Chien AJ, Munster PN, Melisko ME, Rugo HS, Park JW, Goga A, et al. (May 2014). "Phase I dose-escalation study of 5-day intermittent oral lapatinib therapy in patients with human epidermal growth factor receptor 2-overexpressing breast cancer". Journal of Clinical Oncology. 32 (14): 1472–1479. doi:10.1200/JCO.2013.52.1161. PMC 4017711. PMID 24711549.
{{cite journal}}: CS1 maint: overridden setting (link)
- ^ Burris HA, Hurwitz HI, Dees EC, Dowlati A, Blackwell KL, O'Neil B, et al. (August 2005). "Phase I safety, pharmacokinetics, and clinical activity study of lapatinib (GW572016), a reversible dual inhibitor of epidermal growth factor receptor tyrosine kinases, in heavily pretreated patients with metastatic carcinomas". Journal of Clinical Oncology. 23 (23): 5305–5313. doi:10.1200/JCO.2005.16.584. PMID 15955900.
{{cite journal}}: CS1 maint: overridden setting (link)
- ^ Sonnenblick A, de Azambuja E, Agbor-Tarh D, Bradbury I, Campbell C, Huang Y, et al. (August 2016). "Lapatinib-Related Rash and Breast Cancer Outcome in the ALTTO Phase III Randomized Trial". Journal of the National Cancer Institute. 108 (8) djw037. doi:10.1093/jnci/djw037. PMC 5017935. PMID 27098150.
{{cite journal}}: CS1 maint: overridden setting (link)
- ^ "FDA Approval for Lapatinib Ditosylate (Tykerb®)". NCI Cancer Drug Information. Archived from the original on 6 April 2015.
- ^ "Tykerb/Tyverb Phase III gastric cancer study fails to meet primary endpoint". BioPortfolio. Archived from the original on 10 January 2015.
External links
Targeted cancer therapy / antineoplastic agents (L01) |
|---|
| CI monoclonal antibodies ("-mab") | | Receptor tyrosine kinase |
- ErbB: HER1/EGFR (Cetuximab
- Panitumumab)
- HER2/neu (Pertuzumab
- Trastuzumab (+hyaluronidase)
- Trastuzumab emtansine
- Trastuzumab deruxtecan
- Zanidatamab )
|
|---|
| Others for solid tumors |
- EpCAM (Catumaxomab
- Edrecolomab)
- VEGF-A (Bevacizumab)
|
|---|
| Leukemia/lymphoma |
- myeloid: CD33 (Gemtuzumab ozogamicin)
|
|---|
| Other |
- Amivantamab (+hyaluronidase)
- Atezolizumab (+hyaluronidase)
- Avelumab
- Axatilimab
- Belantamab mafodotin
- Bermekimab
- Blinatumomab
- Cemiplimab
- Cosibelimab
- Daratumumab
- Dinutuximab beta
- Dostarlimab
- Durvalumab
- Elotuzumab
- Enfortumab vedotin
- Epcoritamab
- Inotuzumab ozogamicin
- Ipilimumab
- Isatuximab
- Linvoseltamab
- Loncastuximab tesirine
- Mirvetuximab soravtansine
- Mogamulizumab
- Moxetumomab pasudotox
- Naxitamab
- Necitumumab
- Nivolumab (+hyaluronidase, +relatlimab)
- Olaratumab
- Oportuzumab monatox
- Pembrolizumab (+berahyaluronidase alfa)
- Penpulimab
- Polatuzumab vedotin
- Prolgolimab
- Ramucirumab
- Retifanlimab
- Sabatolimab
- Sacituzumab govitecan
- Serplulimab
- Sugemalimab
- Tafasitamab
- Talquetamab
- Tarlatamab
- Teclistamab
- Tislelizumab
- Tisotumab vedotin
- Toripalimab
- Tremelimumab
- Zenocutuzumab
- Zolbetuximab
|
|---|
|
|---|
| Tyrosine kinase inhibitors ("-nib") | | Receptor tyrosine kinase |
- ErbB: HER1/EGFR (Afatinib
- Aumolertinib
- Brigatinib
- Dacomitinib
- Erlotinib
- Gefitinib
- Icotinib
- Lazertinib
- Mobocertinib
- Olmutinib
- Osimertinib
- Rociletinib
- Sevabertinib
- Sunvozertinib
- Vandetanib)
- BRAF
- Dabrafenib
- Encorafenib
- Tovorafenib
- Vemurafenib
- RTK class III: C-kit and PDGFR (Avapritinib
- Axitinib
- Masitinib
- Pazopanib
- Ripretinib
- Sorafenib
- Sunitinib
- Toceranib)
- FLT3 (Lestaurtinib, Gilteritinib (AXL, ALK, LTK))
- VEGFR
- Axitinib
- Cediranib
- Fruquintinib
- Lenvatinib
- Nintedanib
- Pazopanib
- Regorafenib
- Semaxanib
- Sorafenib
- Sunitinib
- Tivozanib
- Toceranib
- Vandetanib
- ALK
- Alectinib
- Brigatinib
- Ceritinib
- Crizotinib
- Ensartinib
- Lorlatinib
- RET inhibitors: Entrectinib (ALK, ROS1, NTRK), Futibatinib (FGFR2), Infigratinib, Larotrectinib (NTRK), Pemigatinib (FGFR), Pralsetinib, Repotrectinib (ROS1, TRK, ALK), Selpercatinib (VEGFR, FGFR), Taletrectinib (ROS1), Vandetanib (VEGFR, EGFR).
- c-MET inhibitors: Cabozantinib (VEGFR), Capmatinib, Crizotinib (ALK)
|
|---|
| Non-receptor |
- Janus kinase (JAK)
- Baricitinib
- Fedratinib
- Filgotinib
- Lestaurtinib
- Momelotinib
- Pacritinib
- Ruxolitinib
- MAP2K (MEK)
- Binimetinib
- Cobimetinib
- Avutometinib (+defactinib)
- Mirdametinib
- Selumetinib
- Trametinib
- EML4-ALK
- Crizotinib
- Entrectinib
- Lorlatinib
- Bruton's (BTK)
- Acalabrutinib
- Ibrutinib
- Orelabrutinib
- Pirtobrutinib
- Rilzabrutinib
- Zanubrutinib
|
|---|
|
|---|
| Other |
- fusion protein against VEGF (Aflibercept)
- proapoptotic peptide against ANXA2 and prohibitin (Adipotide)
- hedgehog inhibitors
- Glasdegib
- Sonidegib
- Vismodegib
- CDK inhibitors
- Abemaciclib
- Dalpiciclib
- Palbociclib
- Ribociclib
- Trilaciclib
- Pi3K inhibitors
- Alpelisib
- Copanlisib
- Duvelisib
- Idelalisib
- Inavolisib
- Parsaclisib
- Fibroblast growth factor receptor (FGFR) inhibitors
- Erdafitinib
- Futibatinib
- Infigratinib
- Pemigatinib
- Avapritinib
- Cabozantinib
- Capivasertib
- Capmatinib
- Defactinib (+avutometinib)
- Entrectinib
- Gilteritinib
- Larotrectinib
- Lenvatinib
- Masitinib
- Midostaurin
- Nintedanib
- Odronextamab
- Pazopanib
- Pexidartinib
- Pralsetinib
- Quizartinib
- Regorafenib
- Repotrectinib
- Ripretinib
- Selpercatinib
- Sitravatinib
- Sorafenib
- Sunitinib
- Surufatinib
- Tebentafusp
- Tepotinib
- Toceranib
- Tunlametinib
- Umbralisib
- Vandetanib
- Venetoclax
- Vimseltinib
|
|---|
Growth factor receptor modulators |
|---|
| Angiopoietin |
- Agonists: Angiopoietin 1
- Angiopoietin 4
- Antagonists: Angiopoietin 2
- Angiopoietin 3
- Kinase inhibitors: Altiratinib
- CE-245677
- Rebastinib
- Antibodies: Evinacumab (against angiopoietin 3)
- Nesvacumab (against angiopoietin 2)
|
|---|
| CNTF |
- Agonists: Axokine
- CNTF
- Dapiclermin
|
|---|
| EGF (ErbB) | EGF
(ErbB1/HER1) |
- Agonists: Amphiregulin
- Betacellulin
- EGF (urogastrone)
- Epigen
- Epiregulin
- Heparin-binding EGF-like growth factor (HB-EGF)
- Murodermin
- Nepidermin
- Transforming growth factor alpha (TGFα)
- Kinase inhibitors: Afatinib
- Agerafenib
- Brigatinib
- Canertinib
- Dacomitinib
- Erlotinib
- Gefitinib
- Grandinin
- Icotinib
- Lapatinib
- Neratinib
- Osimertinib
- Vandetanib
- WHI-P 154
- Antibodies: Cetuximab
- Depatuxizumab
- Depatuxizumab mafodotin
- Futuximab
- Imgatuzumab
- Matuzumab
- Necitumumab
- Nimotuzumab
- Panitumumab
- Zalutumumab
|
|---|
| ErbB2/HER2 |
- Antibodies: Ertumaxomab
- Pertuzumab
- Trastuzumab
- Trastuzumab deruxtecan
- Trastuzumab duocarmazine
- Trastuzumab emtansine
- Kinase inhibitors: Afatinib
- Lapatinib
- Mubritinib
- Neratinib
- Tucatinib
|
|---|
| ErbB3/HER3 |
- Agonists: Neuregulins (heregulins) (1, 2, 6 (neuroglycan C))
- Antibodies: Duligotumab
- Patritumab
- Seribantumab
|
|---|
| ErbB4/HER4 |
- Agonists: Betacellulin
- Epigen
- Heparin-binding EGF-like growth factor (HB-EGF)
- Neuregulins (heregulins) (1, 2, 3, 4, 5 (tomoregulin, TMEFF))
|
|---|
|
|---|
| FGF | | FGFR1 |
- Agonists: Ersofermin
- FGF (1, 2 (bFGF), 3, 4, 5, 6, 8, 10 (KGF2), 20)
- Repifermin
- Selpercatinib
- Trafermin
- Velafermin
|
|---|
| FGFR2 |
- Agonists: Ersofermin
- FGF (1, 2 (bFGF), 3, 4, 5, 6, 7 (KGF), 8, 9, 10 (KGF2), 17, 18, 22)
- Palifermin
- Repifermin
- Selpercatinib
- Sprifermin
- Trafermin
- Antibodies: Aprutumab
- Aprutumab ixadotin
- Kinase inhibitors: Infigratinib
|
|---|
| FGFR3 |
- Agonists: Ersofermin
- FGF (1, 2 (bFGF), 4, 8, 9, 18, 23)
- Selpercatinib
- Sprifermin
- Trafermin
- Antibodies: Burosumab (against FGF23)
|
|---|
| FGFR4 |
- Agonists: Ersofermin
- FGF (1, 2 (bFGF), 4, 6, 8, 9, 19)
- Trafermin
|
|---|
| Unsorted | |
|---|
|
|---|
| HGF (c-Met) |
- Agonists: Fosgonimeton
- Hepatocyte growth factor
- Potentiators: Dihexa (PNB-0408)
- Kinase inhibitors: Altiratinib
- AM7
- AMG-458
- Amuvatinib
- BMS-777607
- Cabozantinib
- Capmatinib
- Crizotinib
- Foretinib
- Golvatinib
- INCB28060
- JNJ-38877605
- K252a
- MK-2461
- PF-04217903
- PF-2341066
- PHA-665752
- SU-11274
- Tivantinib
- Volitinib
- Antibodies: Emibetuzumab
- Ficlatuzumab
- Flanvotumab
- Onartuzumab
- Rilotumumab
- Telisotuzumab
- Telisotuzumab vedotin
|
|---|
| IGF | | IGF-1 |
- Agonists: des(1-3)IGF-1
- Insulin-like growth factor-1 (somatomedin C)
- IGF-1 LR3
- Insulin-like growth factor-2 (somatomedin A)
- Insulin
- Mecasermin
- Mecasermin rinfabate
- Kinase inhibitors: BMS-754807
- Linsitinib
- NVP-ADW742
- NVP-AEW541
- OSl-906
- Antibodies: AVE-1642
- Cixutumumab
- Dalotuzumab
- Figitumumab
- Ganitumab
- Robatumumab
- R1507
- Teprotumumab
- Xentuzumab (against IGF-1 and IGF-2)
|
|---|
| IGF-2 |
- Agonists: Insulin-like growth factor-2 (somatomedin A)
- Antibodies: Dusigitumab
- Xentuzumab (against IGF-1 and IGF-2)
|
|---|
| Others |
- Binding proteins: IGFBP (1, 2, 3, 4, 5, 6, 7)
- Cleavage products/derivatives with unknown target: Glypromate (GPE, (1-3)IGF-1)
- Trofinetide
|
|---|
|
|---|
| LNGF (p75NTR) |
- Agonists: BDNF
- BNN-20
- BNN-27
- Cenegermin
- DHEA
- DHEA-S
- NGF
- NT-3
- NT-4
- Antibodies: Against NGF: ABT-110 (PG110)
- ASP-6294
- Fasinumab
- Frunevetmab
- Fulranumab
- MEDI-578
- Ranevetmab
- Tanezumab
- Aptamers: Against NGF: RBM-004
- Decoy receptors: LEVI-04 (p75NTR-Fc)
|
|---|
| PDGF |
- Agonists: Becaplermin
- Platelet-derived growth factor (A, B, C, D)
- Kinase inhibitors: Agerafenib
- Avapritinib
- Axitinib
- Crenolanib
- Imatinib
- Lenvatinib
- Masitinib
- Motesanib
- Nintedanib
- Pazopanib
- Radotinib
- Quizartinib
- Ripretinib
- Sunitinib
- Sorafenib
- Toceranib
- Antibodies: Olaratumab
- Ramucirumab
- Tovetumab
|
|---|
| RET (GFL) | | GFRα1 |
- Agonists: Glial cell line-derived neurotrophic factor (GDNF)
- Liatermin
- Kinase inhibitors: Vandetanib
|
|---|
| GFRα2 |
- Agonists: Neurturin (NRTN)
- Kinase inhibitors: Vandetanib
|
|---|
| GFRα3 |
- Kinase inhibitors: Vandetanib
|
|---|
| GFRα4 |
- Agonists: Persephin (PSPN)
- Kinase inhibitors: Vandetanib
|
|---|
| Unsorted |
- Kinase inhibitors: Agerafenib
|
|---|
|
|---|
| SCF (c-Kit) |
- Agonists: Ancestim
- Stem cell factor
|
|---|
| TGFβ | |
|---|
| Trk | | TrkA |
- Positive allosteric modulators: ACD856
- ACD857
- Ponazuril (ACD855)
- Toltrazuril
- Negative allosteric modulators: VM-902A
- Kinase inhibitors: Altiratinib
- AZD-6918
- CE-245677
- CH-7057288
- DS-6051
- Entrectinib
- GZ-389988
- K252a
- Larotrectinib
- Lestaurtinib
- Milciclib
- ONO-4474
- ONO-5390556
- PLX-7486
- Rebastinib
- SNA-120 (pegylated K252a))
- Antibodies: Against TrkA: GBR-900; Against NGF: ABT-110 (PG110)
- ASP-6294
- Fasinumab
- Frunevetmab
- Fulranumab
- MEDI-578
- Ranevetmab
- Tanezumab
- Aptamers: Against NGF: RBM-004
- Decoy receptors: ReN-1820 (TrkAd5)
|
|---|
| TrkB |
- Agonists: 3,7-DHF
- 3,7,8,2'-THF
- 4'-DMA-7,8-DHF
- 7,3'-DHF
- 7,8-DHF
- 7,8,2'-THF
- 7,8,3'-THF
- Amitriptyline
- Braegen-02
- BDNF
- BNN-20
- Deoxygedunin
- Diosmetin
- DMAQ-B1
- HIOC
- LM22A-4
- N-Acetylserotonin
- NT-3
- NT-4
- Norwogonin (5,7,8-THF)
- R7
- R13 (BrAD-R13, Braegen-01)
- TDP6
- Antagonists: ANA-12
- Cyclotraxin B
- Gossypetin (3,5,7,8,3',4'-HHF)
- Positive allosteric modulators: ACD856
- ACD857
- Ponazuril (ACD855)
- Toltrazuril
- Kinase inhibitors: Altiratinib
- AZD-6918
- CE-245677
- CH-7057288
- DS-6051
- Entrectinib
- GZ-389988
- K252a
- Larotrectinib
- Lestaurtinib
- ONO-4474
- ONO-5390556
- PLX-7486
|
|---|
| TrkC |
- Agonists: BNN-20
- DHEA
- NT-3
- Positive allosteric modulators: ACD856
- Kinase inhibitors: Altiratinib
- AZD-6918
- CE-245677
- CH-7057288
- DS-6051
- Entrectinib
- GZ-389988
- K252a
- Larotrectinib
- Lestaurtinib
- ONO-4474
- ONO-5390556
- PLX-7486
|
|---|
|
|---|
| VEGF |
- Agonists: Placental growth factor (PGF)
- Ripretinib
- Telbermin
- VEGF (A, B, C, D (FIGF))
- Allosteric modulators: Cyclotraxin B
- Kinase inhibitors: Agerafenib
- Altiratinib
- Axitinib
- Cabozantinib
- Cediranib
- Fruquintinib
- Lapatinib
- Lenvatinib
- Motesanib
- Nintedanib
- Pazopanib
- Pegaptanib
- Rebastinib
- Regorafenib
- Semaxanib
- Sorafenib
- Sunitinib
- Toceranib
- Tivozanib
- Vandetanib
- WHI-P 154
- Antibodies: Alacizumab pegol
- Bevacizumab
- Icrucumab
- Ramucirumab
- Ranibizumab
- Decoy receptors: Aflibercept
|
|---|
| Others |
- Additional growth factors: Adrenomedullin
- Colony-stimulating factors (see here instead)
- Connective tissue growth factor (CTGF)
- Ephrins (A1, A2, A3, A4, A5, B1, B2, B3)
- Erythropoietin (see here instead)
- Glucose-6-phosphate isomerase (GPI; PGI, PHI, AMF)
- Glia maturation factor (GMF)
- Hepatoma-derived growth factor (HDGF)
- Interleukins/T-cell growth factors (see here instead)
- Leukemia inhibitory factor (LIF)
- Macrophage-stimulating protein (MSP; HLP, HGFLP)
- Midkine (NEGF2)
- Migration-stimulating factor (MSF; PRG4)
- Oncomodulin
- Pituitary adenylate cyclase-activating peptide (PACAP)
- Pleiotrophin
- Renalase
- Thrombopoietin (see here instead)
- Wnt signaling proteins
- Additional growth factor receptor modulators: Cerebrolysin (neurotrophin mixture)
|
|---|
GSK |
|---|
| Subsidiaries | | Current |
- GlaxoSmithKline Pakistan
- GlaxoSmithKline Pharmaceuticals Ltd
- Stiefel Laboratories
- Tesaro
- ViiV Healthcare (85%)
|
|---|
| Former | Haleon |
|---|
|
|---|
Predecessors,
acquisitions |
- Allen & Hanburys
- Beecham Group
- Block Drug
- Burroughs Wellcome
- Glaxo
- Glaxo Wellcome
- Human Genome Sciences
- Recherche et Industrie Thérapeutiques
- Reliant Pharmaceuticals
- S. E. Massengill Company
- SmithKline Beecham
- Smith, Kline & French
|
|---|
| Products | | Current | | Pharma | |
|---|
| Vaccines |
- Arexvy
- Bexsero
- Boostrix
- Cervarix
- Engerix-B
- Fluarix
- FluLaval
- Havrix
- Hepatyrix
- Hiberix
- Infanrix
- H5N1 vaccine
- Kinrix
- Menveo
- Pandemrix
- Pediarix
- Rabavert
- Rotarix
- Shingrix
- Twinrix … more
|
|---|
|
|---|
| Former |
- Actifed
- Advil
- Aquafresh
- BC Powder
- Biotene
- Caltrate
- Centrum
- ChapStick
- Emergen-C
- Eno
- Excedrin
- Flonase
- Geritol
- Goody's Powder
- Horlicks
- Lucozade
- Nicoderm
- Nicorette
- NiQuitin
- Parodontax
- Ribena
- Sensodyne
- Tums
|
|---|
|
|---|
| People | Board of
Directors |
- Philip Hampton
- Emma Walmsley
- Simon Dingemans
- Roy M. Anderson
- Manvinder Banga
- Patrick Vallance
- Vivienne Cox
- Lynn Elsenhans
- Jesse Goodman
- Judy Lewent
- Urs Rohner
- Laurie Glimcher
|
|---|
| Other |
- Thomas Beecham
- Silas M. Burroughs
- Mahlon Kline
- John K. Smith
- Henry Wellcome
- Andrew Witty
- Chris Gent
|
|---|
|
|---|
| Litigation |
- Canada v. GlaxoSmithKline Inc.
- Christopher v. SmithKline Beecham Corp.
- GlaxoSmithKline Services Unlimited v Commission
- United States v. Glaxo Group Ltd.
- United States v. GlaxoSmithKline
|
|---|
| Other |
- Drug Industry Documents Archive
- GlaxoSmithKline Prize
- Side Effects
- Study 329
|
|---|
 Category Category
|
